Estrogen is one of the most important hormones in the female body. It shapes reproductive health, bone strength, cardiovascular function, skin quality, and mood. When estrogen levels fall — due to aging, menopause, or lifestyle factors — women can experience a wide range of uncomfortable symptoms. The good news is that there are proven, natural ways to increase estrogen levels and support overall hormonal balance. This guide explores how to boost estrogen naturally through diet, lifestyle changes, and targeted supplements — whether you are in perimenopause, postmenopause, or simply looking to raise estrogen naturally.
What Is Estrogen and Why Does It Matter?
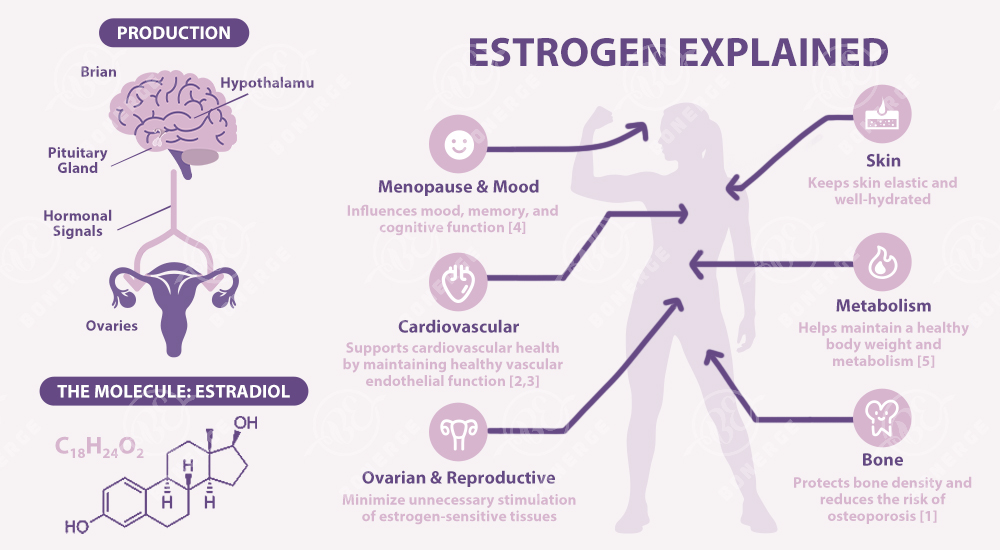
Figure 1. Estrogen production pathway and its key physiological roles in women
Estrogen is a group of sex hormones — primarily estradiol (E2), estrone (E1), and estriol (E3) — produced mainly by the ovaries, with smaller amounts made by the adrenal glands and adipose tissue. Beyond reproduction, estrogen also:
Protects bone density and reduces the risk of osteoporosis[1]
Supports cardiovascular health by maintaining healthy vascular endothelial function[2,3]
Keeps skin elastic and well-hydrated
Helps maintain a healthy body weight and metabolism[5]
When estrogen levels fall too low, women may experience hot flashes, night sweats, vaginal dryness, mood swings, fatigue, brain fog, and joint pain. Learning how to increase estrogen levels naturally is therefore not just about managing symptoms — it is about protecting long-term health.[4]
Estrogen and Menopause: What Is the Connection?
Menopause is clinically defined as 12 consecutive months without menstruation, typically occurring between ages 45 and 55, and marks the permanent end of the ovaries' reproductive function.[5,6] The transition leading up to menopause — perimenopause — is marked by fluctuating and declining estrogen levels. The core biological driver is follicular depletion: as the ovaries exhaust their egg supply, estradiol production drops below 20 pg/mL, while FSH and LH levels rise sharply due to loss of negative feedback on the hypothalamic-pituitary-ovarian (HPO) axis.
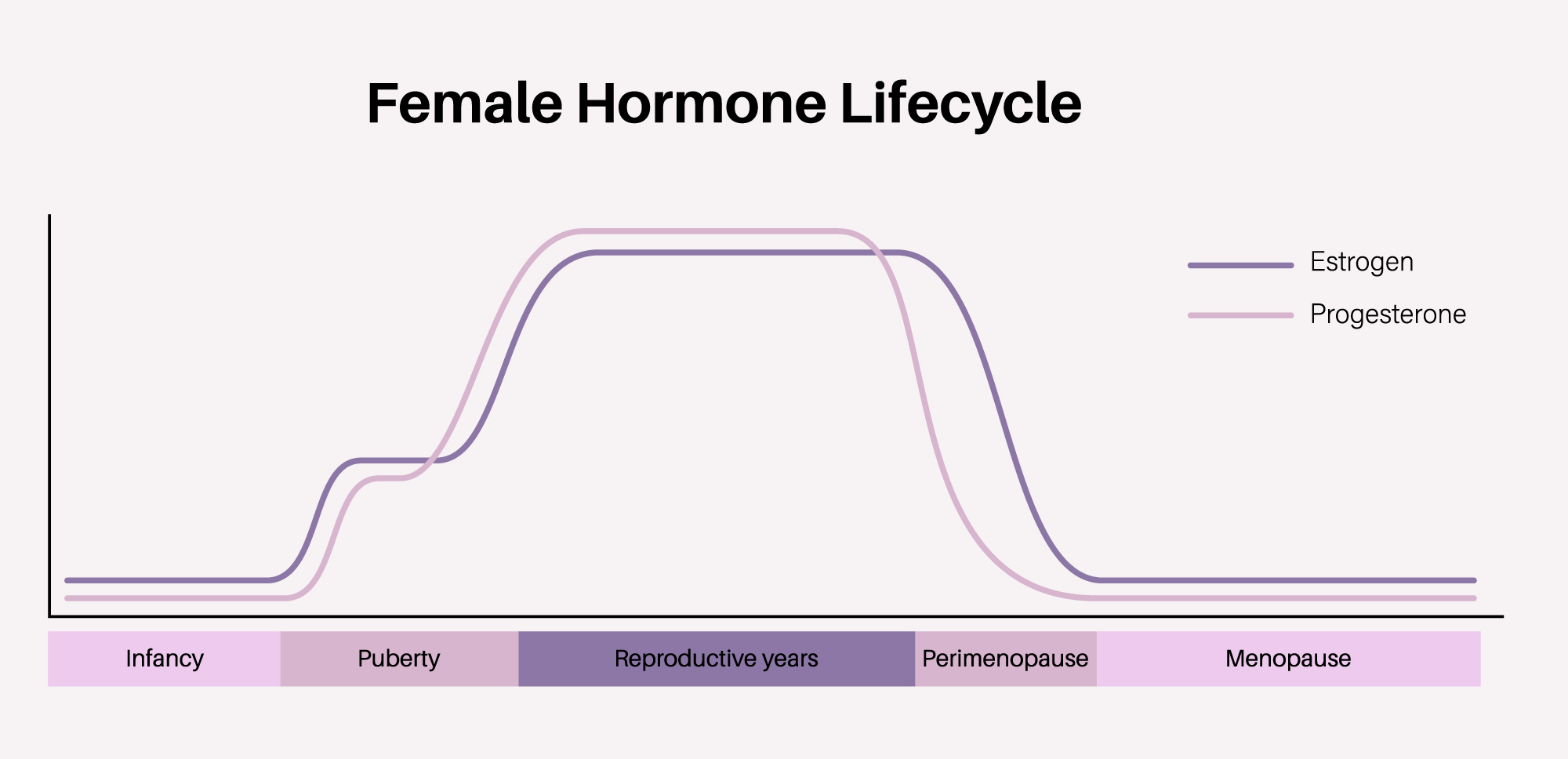
Figure 2. Estrogen and progesterone levels across the female lifecycle, from puberty through reproductive years to the sharp hormonal decline of perimenopause and menopause.
This hormonal disruption produces a wide spectrum of symptoms. The most common postmenopausal symptoms of low estrogen include:
Vasomotor symptoms: hot flashes, night sweats, and heart palpitations (affecting up to 91.7% of women) [4]
Genitourinary symptoms: vaginal dryness, urinary urgency, and painful intercourse [5]
Psychological symptoms: anxiety, depression, irritability, and poor sleep [4]
Musculoskeletal: joint pain, muscle loss, and accelerated bone loss — postmenopausal bone density can drop up to 20% within five years [1]
Cardiovascular risk: estrogen deficiency impairs vascular endothelial function, raising atherosclerosis risk two- to three-fold after menopause [2,3]
Understanding this estrogen-menopause connection is the first step toward finding evidence-based strategies to raise estrogen naturally or explore appropriate medical support.
How Can I Raise My Estrogen Levels Naturally
If you are wondering how to increase estrogen naturally in females, the answer lies in a multi-layered approach: supporting production, optimizing metabolism, and building a hormone-friendly lifestyle. Here are the most effective natural ways to increase estrogen.
1. Eat Estrogen-Rich Foods (Phytoestrogens)
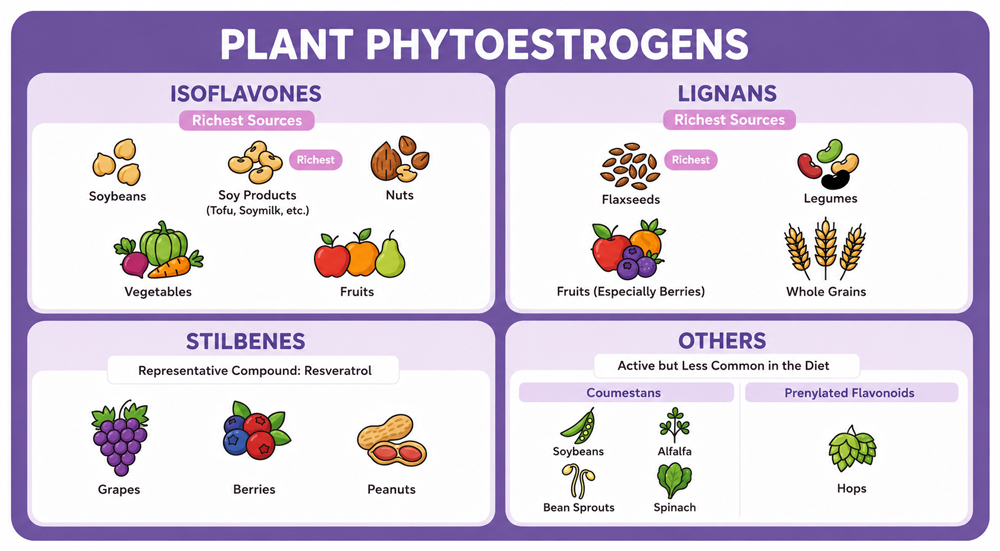
Figure 3. Major categories of plant phytoestrogens and their primary dietary sources, including isoflavones, lignans, stilbenes, and coumestans.
Phytoestrogens are plant compounds that bind to estrogen receptors (ERα and ERβ) and exert weak estrogenic or antiestrogenic effects depending on the body's circulating estrogen level — acting more estrogenically when estrogen is low.[10] This makes estrogen-rich foods particularly relevant for perimenopausal and postmenopausal women. Key foods that boost estrogen include:
Soy foods: tofu, tempeh, edamame, soy milk — rich in isoflavones (genistein and daidzein) [10]
Flaxseeds: the richest dietary source of lignans, a type of phytoestrogen shown to support hormonal balance [11]
Legumes: chickpeas, lentils, and beans — contain moderate phytoestrogens and beneficial fiber
Whole grains: oats, barley, and wheat bran contain lignans [11]
Vegetables: broccoli, kale, Brussels sprouts, garlic — support estrogen metabolism [14]
Fruits: peaches, dried apricots, strawberries, and prunes — estrogen-producing foods rich in flavonoids
Nuts and seeds: sesame seeds, sunflower seeds, walnuts, and pistachios
Including a variety of foods containing natural estrogen in your daily diet is one of the simplest ways to increase estrogen food-based hormonal support. See the table below for a quick overview.
Table 1: Top Estrogen-Rich Foods and Their Phytoestrogen Levels
Food Category | Top Examples | Estrogen-Boosting Level |
Soy & Legumes | Tofu, edamame, soy milk, tempeh, lentils, chickpeas | Very High (isoflavones: genistein, daidzein) |
Seeds | Flaxseeds, sesame seeds, sunflower seeds | High (lignans, phytoestrogens) |
Whole Grains | Oats, barley, wheat bran, brown rice | Moderate (lignans) |
Fruits | Peaches, strawberries, dried apricots, dried prunes | Moderate (flavonoids, phytoestrogens) |
Vegetables | Garlic, onions, broccoli, Brussels sprouts, kale | Moderate (isoflavones, indoles) |
Nuts | Pistachios, walnuts, peanuts, cashews | Moderate (phytosterols, lignans) |
Beverages | Green tea, red clover tea, soy milk | Low – Moderate |
2. Maintain a Balanced, Nutrient-Dense Diet
Estrogen is synthesized from cholesterol. Extremely low-fat diets can deplete the raw material the body needs to produce hormones.[12]To naturally increase estrogen, focus on:
Adequate healthy fats: olive oil, avocados, fatty fish, and nuts
Sufficient protein: eggs, poultry, legumes, and dairy to support enzymatic processes
Key micronutrients: zinc, magnesium, B vitamins, and vitamin D — all involved in hormone synthesis and metabolism
Fiber-rich foods: dietary fiber supports the liver's clearance of used estrogens and limits their reabsorption in the gut
3. Support Your Liver and Gut Health
Estrogen is not just produced — it is also metabolized and eliminated. The liver conjugates used estrogens for excretion, while the gut microbiome contains a collection of bacterial genes called the 'estrobolome,' which regulates whether conjugated estrogens are excreted or deconjugated and reabsorbed into circulation. Disruption to either system can alter circulating estrogen levels. Practical strategies include:
Eat cruciferous vegetables such as broccoli, cauliflower, and kale — they contain indole-3-carbinol (I3C) and diindolylmethane (DIM), compounds that induce cytochrome P450 enzymes and support healthy estrogen metabolism in the liver [14]
Consume fermented foods (yogurt, kefir, kimchi, natto) to maintain gut microbiome diversity, which is associated with better estrogen regulation [13]
Limit alcohol: the liver prioritizes alcohol metabolism, which impairs estrogen clearance [12]
Eat prebiotic-rich foods (garlic, onions, asparagus, oats) to nourish beneficial gut bacteria
4. Exercise Regularly — But Avoid Overtraining
Regular moderate exercise supports hormonal balance by improving insulin sensitivity, reducing excess body fat, and lowering chronic stress hormones.[15,16] However, excessive high-intensity training combined with insufficient caloric intake can suppress the HPO axis and reduce estrogen production. The recommended approach is at least 150 minutes of moderate aerobic activity per week combined with two sessions of resistance training.
5. Manage Stress and Prioritize Sleep
Chronic stress elevates cortisol, which can disrupt HPO axis signaling and reduce estrogen output. Poor sleep further disrupts circadian hormonal rhythms. To get estrogen naturally and sustainably:
Practice mindfulness, yoga, or meditation to lower chronic cortisol levels
Aim for 7–9 hours of quality sleep each night
Maintain a consistent sleep schedule and limit evening screen exposure
6. Maintain a Healthy Body Weight
Adipose tissue converts androgens to estrogens through aromatization. Very low body weight suppresses estrogen production, while excessive adiposity can cause hormonal dysregulation. Maintaining a healthy BMI supports optimal estrogen balance. [15]
7. Reduce Endocrine-Disrupting Chemical Exposure
Synthetic chemicals such as BPA, phthalates, and parabens can mimic or block estrogen signaling. Practical steps include avoiding plastic containers for heating food, choosing glass or stainless steel water bottles, and selecting fragrance-free personal care products where possible.[12]
Supplements That Help Boost Estrogen and Ease Menopause Symptoms
In addition to diet and lifestyle changes, certain natural estrogen supplements may help support hormonal balance and relieve menopause-related symptoms. These are not a replacement for menopausal hormone therapy (MHT) — they work more gently and are generally safe for healthy women. Always consult a healthcare provider before starting any new supplement.
Black Cohosh
One of the most researched natural estrogen replacement therapy options, black cohosh (Cimicifuga racemosa) has been evaluated across large clinical datasets. A 2021 meta-analysis and review comprising over 43,000 women found isopropanolic black cohosh extract (iCR) to be significantly superior to placebo for reducing menopausal vasomotor symptoms.[17] It appears to work via serotonin receptor modulation rather than direct estrogenic activity.
Red Clover Isoflavones
Red clover is rich in isoflavones — the same family of phytoestrogens found in soy. It is widely used as a natural estrogen therapy to reduce hot flashes. A systematic review and meta-analysis (12 RCTs, 533 participants) found soy isoflavones effective for alleviating menopausal symptoms (Hedges' g = −0.25, p = 0.004).[10]
S-Equol
S-equol is a naturally occurring metabolite of the soy isoflavone daidzein, produced by specific intestinal bacteria. Unlike daidzein itself, S-equol binds selectively and with high affinity to estrogen receptor β (ERβ) — the receptor subtype associated with bone, cardiovascular, and neurological protection — while showing little activity at ERα, which is linked to breast and uterine tissue stimulation.[21] This selective ERβ binding gives S-equol a distinct advantage over conventional phytoestrogens: potential estrogenic benefits without the hormonal risks associated with ERα activation.
A key challenge is that S-equol is not widely present in food — it must be synthesized by gut bacteria from daidzein following soy consumption. However, only approximately 50% of Asians and 25% of non-Asians carry the intestinal bacteria capable of this conversion, meaning many women cannot generate S-equol naturally and may not respond to standard soy isoflavone supplements.Direct S-equol supplementation offers a practical solution for these non-producers.
A systematic review and meta-analysis of randomized clinical trials (6 studies, 779 participants) found that S-equol supplementation in equol non-producers significantly reduced the incidence and severity of hot flashes, with a significant overall benefit on hot flash scores and a generally low risk of bias. The standard dose used in most trials is 10 mg per day (5 mg twice daily), in line with S-equol's half-life of 7–10 hours. A 12-week trial (n = 247) reported that 90% of women noticed improvement in at least one menopausal symptom, with 82% reporting fewer hot flashes and 71% reporting reduced night sweats.[22]
Emerging evidence also suggests S-equol may support bone density and cardiovascular health in postmenopausal women. Current safety data do not raise concerns regarding breast or endometrial tissue — a meaningful distinction from estrogen-based therapies — though women with a personal or family history of hormone-sensitive cancers should consult their healthcare provider before use.
Maca Root
Maca (Lepidium meyenii) is an Andean adaptogenic root that does not contain estrogen but supports the body's own hormone production. A double-blind, crossover clinical pilot study in perimenopausal women found that maca supplementation produced statistically significant changes in estradiol (E2), FSH, and LH levels, along with improved Kupperman Menopausal Index scores.[18]
Evening Primrose Oil
Rich in gamma-linolenic acid (GLA), evening primrose oil may help manage hot flashes and breast tenderness. It is a popular natural way to increase estrogen support among menopausal women, though large-scale clinical evidence remains limited.
Omega-3 Fatty Acids
Found in fatty fish, flaxseeds, and fish oil supplements, omega-3 fatty acids support cardiovascular health, reduce inflammation, and may ease mood-related symptoms of low estrogen. A 2023 systematic review concluded that omega-3 PUFA supplementation shows variable benefit on vasomotor symptoms, with some trials reporting reductions in hot flash frequency and intensity.[19]
Vitamin D and Calcium
While not directly estrogenic, vitamin D and calcium are critical for bone protection when estrogen falls. Postmenopausal women are generally advised to aim for 800–1000 IU of vitamin D3 daily along with 1200 mg of calcium from food and/or supplements.[20]
When Should You See a Doctor?
Natural strategies are an excellent first step for mild to moderate symptoms. However, if symptoms severely affect daily life — or if you have concerns about bone health or cardiovascular risk — speak with a healthcare provider. Menopausal hormone therapy (MHT), also called HRT, remains the most effective medical treatment for moderate-to-severe symptoms. Clinical evidence shows it can reduce hot flash frequency by approximately 80% and lower fracture risk by around 30%.[6,7] Transdermal estrogen formulations carry significantly lower thrombotic risk than oral forms.[8] Your provider can help you weigh the individual benefits and risks, including breast cancer considerations.[9]
Conclusion
Knowing how to naturally increase estrogen does not require drastic changes. By incorporating foods high in estrogen into your daily diet, supporting your liver and gut health, managing stress, exercising wisely, and choosing targeted natural estrogen supplements, you can take meaningful steps toward hormonal balance. Whether you want to raise estrogen naturally during perimenopause, address postmenopausal symptoms of low estrogen, or simply boost estrogen through everyday choices, a consistent and holistic approach is key. If symptoms persist or worsen, always seek professional guidance.
This article is for informational purposes only and does not constitute medical advice. Please consult a qualified healthcare provider before starting any new supplement or treatment regimen.
References:
[1] Lubkowska A, Dobek A, Mieszkowski J, et al. Adiponectin as a biomarker of osteoporosis in postmenopausal women: Controversies. Disease Markers. 2014;2014:1–14. https://doi.org/10.1155/2014/975178
[2] Sabbatini AR, Kararigas G. Menopause-related estrogen decrease and the pathogenesis of HFpEF. Journal of the American College of Cardiology. 2020;75(9):1074–1082. https://doi.org/10.1016/j.jacc.2019.11.069
[3] Vaccarezza M, Papa V, Milani D, et al. Sex/gender-specific imbalance in CVD: Could physical activity help to improve clinical outcome targeting CVD molecular mechanisms in women? International Journal of Molecular Sciences. 2020;21(4):1477. https://doi.org/10.3390/ijms21041477
[4] D'Angelo S, Bevilacqua G, Hammond J, et al. Impact of menopausal symptoms on work: Findings from women in the HEAF study. International Journal of Environmental Research and Public Health. 2022;20(1):295. https://doi.org/10.3390/ijerph20010295
[5] Motlani V, Motlani G, Pamnani S, et al. Changed endocrinology in postmenopausal women: A comprehensive view. Cureus. 2023. https://doi.org/10.7759/cureus
[6] Academic Committee of the Korean Society of Menopause; Lee SR, Cho MK, et al. The 2020 menopausal hormone therapy guidelines. Journal of Menopausal Medicine. 2020;26(2):69. https://doi.org/10.6118/jmm.20000
[7] Hickey M, Elliott J, Davison SL. Hormone replacement therapy. BMJ. 2012;344:e763. https://doi.org/10.1136/bmj.e763
[8] Flores VA, Pal L, Manson JE. Hormone therapy in menopause: Concepts, controversies, and approach to treatment. Endocrine Reviews. 2021;42(6):720–752. https://doi.org/10.1210/endrev/bnab011
[9] Martins SC, Araújo MAM, Moura JPM, et al. Hormone therapy and breast cancer: A literature review about the influence of hormonal treatment on neoplastic development. Revista Médica de Minas Gerais. 2021;31. https://doi.org/10.5935/2238-3182.20210022
[10] Seki R, Miyagawa K, Masuda K, et al. Effects of soy isoflavones on menopausal symptoms in perimenopausal women: A systematic review and meta-analysis. Frontiers in Nutrition. 2025. PMC12296567. https://doi.org/10.3389/fnut.2025
[11] Ghazanfarpour M, Sadeghi R, Roudsari RL, et al. Effects of flaxseed and Hypericum perforatum on hot flash, vaginal atrophy and estrogen-dependent cancers in menopausal women: A systematic review and meta-analysis. Avicenna Journal of Phytomedicine. 2016;6(3):273–283. PMC4930534.
[12] Erdélyi A, Pálfi E, Tűű L, et al. The importance of nutrition in menopause and perimenopause — a review. Nutrients. 2023;16(1):27. https://doi.org/10.3390/nu16010027
[13] Peters BA, Lin J, Qi Q, et al. Menopause is associated with an altered gut microbiome and estrobolome, with implications for adverse cardiometabolic risk. mSystems. 2022;7:e0027322. PMC9239235. https://doi.org/10.1128/msystems.00273-22
[14] Auborn KJ, Fan S, Rosen EM, et al. Indole-3-carbinol is a negative regulator of estrogen. Journal of Nutrition. 2003;133(7 Suppl):2470S–2475S. https://doi.org/10.1093/jn/133.7.2470S
[15] Barrell A. Perimenopause and menopause: An opportunity to engage, inform, and empower women to live well. European Medical Journal. 2023:47–53.
[16] Trémollieres FA, Chabbert-Buffet N, Plu-Bureau G, et al. Management of postmenopausal women: CNGOF and GEMVi clinical practice guidelines. Maturitas. 2022;163:62–81. https://doi.org/10.1016/j.maturitas.2021.12.007
[17] Castelo-Branco C, Gambacciani M, Cano A, et al. Review & meta-analysis: Isopropanolic black cohosh extract iCR for menopausal symptoms — an update on the evidence. Climacteric. 2021;24(2):109–119. https://doi.org/10.1080/13697137.2020.1820477
[18] Meissner HO, Reich-Bilinska H, Mscisz A, Kedzia B. Therapeutic effects of pre-gelatinized Maca (Lepidium peruvianum Chacon) used as a non-hormonal alternative to HRT in perimenopausal women — clinical pilot study. International Journal of Biomedical Science. 2006;2(2):143–159. PMC3614596.
[19] Iqbal AZ, Wu SK, Zailani H, et al. Effects of omega-3 polyunsaturated fatty acids intake on vasomotor symptoms, sleep quality and depression in postmenopausal women: A systematic review. Nutrients. 2023;15(19):4231. PMC10574492. https://doi.org/10.3390/nu15194231
[20] Lang Y. Ten health care tasks for women during menopause. Health Guide. 2015;21(5):38.
[21] Sekikawa A, Weaver A, Mroz K, et al. S-Equol as a gut-derived phytoestrogen targeting estrogen receptor beta: A promising bioactive nutrient for bone health in aging women and men. Nutrients. 2025;17(24):3962. PMC12735577. https://doi.org/10.3390/nu17243962 [Also drawing on: Messina M. Soy and Health Update: Evaluation of the Clinical and Epidemiologic Literature. Nutrients. 2016;8(12):754.]
[22] Rowland I, Faughnan M, Hoey L, et al. Equol decreases hot flashes in postmenopausal women: A systematic review and meta-analysis of randomized clinical trials. Journal of Medicinal Food. 2019;22(2):127–139. https://doi.org/10.1089/jmf.2018.4265




































 Time:May 09, 2026
Time:May 09, 2026
 Share:
Share:











 +1(425)866-9043
+1(425)866-9043
 sales@bonerge.com
sales@bonerge.com