Tossing and turning at 2 a.m., you reach for your melatonin bottle again. You hope tonight will be different, but hours pass and you’re still awake. You’re not alone. Millions of people have trouble sleeping.
Using only single-ingredient supplements, like melatonin, often disappoints. Insomnia is not a one-size-fits-all problem. It stems from breakdowns in multiple body systems.
In this article, we’ll break down the four core biological reasons your sleep problems persist. We’ll debunk common myths about sleep supplements and explain why effective sleep support needs a system repair mindset, not just a quick fix.
We’ll also look at the growing sleep supplement market. We’ll cover the shift to natural, multi-targeted solutions. These solutions fix root causes, not just symptoms.

The Global Sleep Crisis: Key Facts
The Science of Sleep: How Is Sleep Regulated?
Sleep disturbances have grown from a minor annoyance to a global public health issue. Clinical research shows that 10% of adults live with chronic insomnia, while another 20% experience occasional sleep problems that disrupt daily life[1]. For individuals with anxiety, the connection is even stronger, as sleep–wake dysregulation commonly co-occurs due to shared neural circuit mechanisms[2].
This trend is not only observed in clinical settings but also confirmed at the population level.The 6th Global Sleep Survey by ResMed, covering 30,000 respondents across 13 countries, further highlights the scale of the problem. More than half (53%) reported getting good sleep on four nights or fewer per week, while fewer than one-third sleep well every night. Sleep difficulties are rising across both genders, with 48% of women reporting trouble falling asleep, up from 38% the previous year, and men showing a similar increase from 29% to 42%[3].
The Sleep Supplement Market: Growth and Limits
The global sleep supplement market is valued at approximately $7.5 billion in 2025 and is projected to exceed $12–13 billion by the mid-2030s, with a CAGR of around 5.4%[15]. Melatonin remains one of the most widely used sleep ingredients, reflecting strong consumer demand for natural sleep aids. At the same time, the Asia-Pacific region is expected to be the fastest-growing market, driven by rising stress levels and increasing health awareness[4].
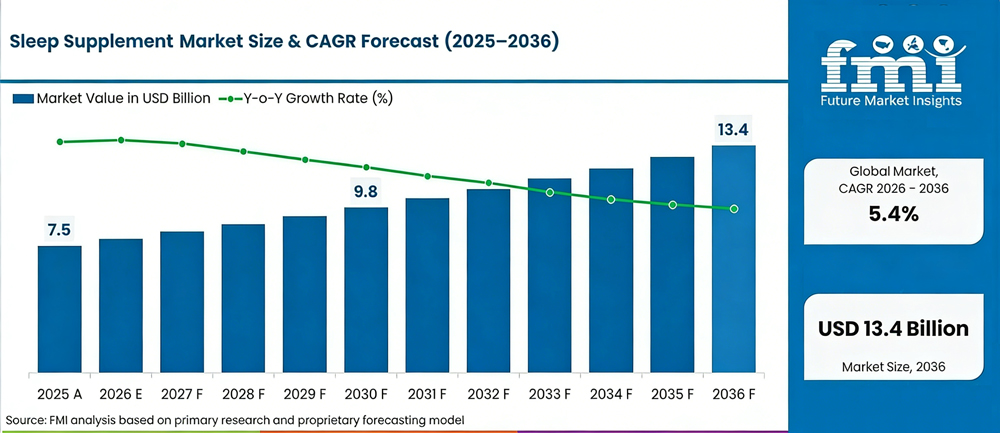
Figure 1. Global sleep supplement market size and growth forecast, 2025–2036 (Source: Future Market Insights, 2025).
However, growing awareness has not translated into better sleep outcomes. According to the ResMed Global Sleep Survey, more than half of respondents report poor sleep quality, and sleep & stress remain deeply connected — anxiety and chronic tension are now the leading causes of sleep disturbances worldwide.
This highlights a critical gap: while the market is growing, many solutions still fail to address the underlying biological complexity of sleep disorders. Most products focus on single targets, whereas chronic insomnia is often driven by multiple interconnected systems.
Mechanism 1: Melatonin Receptor Dysfunction
Common Myth: Poor sleep means low melatonin levels. Core Reality: The problem is rarely how much melatonin you make, but how well your cells receive its signal.
Melatonin, the hormone your brain releases at night, regulates your sleep-wake cycle. But melatonin doesn't act alone — it only works when it binds to two specific receptors in the brain: MT1 and MT2. Think of melatonin as a key and these receptors as locks. When the locks are damaged or desensitized, even a flood of melatonin won't open the door to restful sleep.
Two factors can silently impair how well your receptors work. First, taking supplemental melatonin in doses higher than your body naturally produces may cause receptors to downregulate over time — becoming less responsive to the signal. Second, chronic stress disrupts circadian rhythm at the hormonal level, interfering with the precise timing melatonin needs to bind effectively to MT1 and MT2 receptors. Both factors shift the problem away from how much melatonin you have, and toward how well your cells can receive it.
MT1 Receptors: Primarily located within the brain’s internal clock, these receptors synchronize the body with nocturnal signals to initiate the sleep process. Dysfunction within the MT1 pathway leads to significant sleep-onset difficulties or disrupted circadian rhythms.[4]
MT2 Receptors: Located in the thalamus, they help you get deep sleep and truly restorative rest. Activating MT2 receptors boosts slow-wave sleep — the phase that repairs your body and mind, and is essential for healthy sleep and wakefulness the next day.[5]
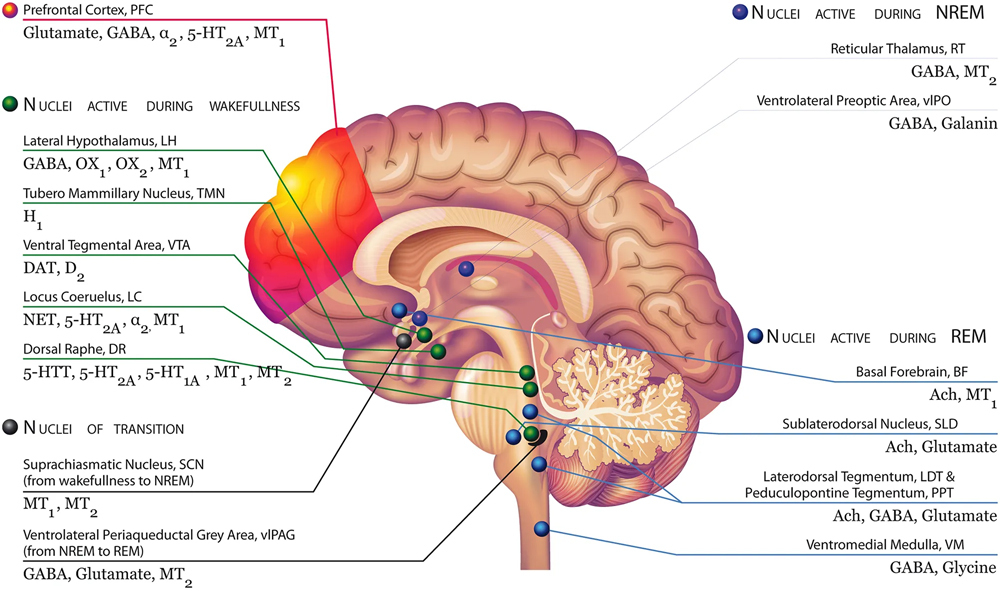
Figure 2. Brain regions and neurotransmitters governing sleep-wake regulation, including key MT₁ and MT₂ receptor sites.[4]
Why Melatonin Stops Working
Taking melatonin long-term makes your cells less responsive to it, so the supplement loses effectiveness over time. Stress, anxiety, and too much blue light also damage MT1 and MT2 receptors[5]. In these cases, taking more melatonin won’t fix the real problem: your cells can’t “hear” the sleep signal.
Mechanism 2: The GABA and Gut-Brain Axis Block
Common Myth: Feeling tense means low GABA levels.Core Reality: Your brain’s calm pathway might be blocked, and the root cause could be in your gut.
GABA is your brain’s main “calming” chemical, slowing nerve activity to help you relax[6]. For years, people took GABA supplements to fix low levels, but science shows oral GABA struggles to cross the blood-brain barrier. Any effects you feel often come from calming your body, not your brain.
Clinical reviews find only limited evidence that oral GABA supplements improve sleep — a gap researchers attribute primarily to uncertainty over whether supplemental GABA can cross the blood-brain barrier in meaningful amounts.[7]
The "Second Brain" Breakthrough: The Gut-Brain Axis
Recent research has revealed another critical pathway — the gut-brain axis. Studies show that certain gut probiotics, such as Lactobacillus plantarum Lp815, can synthesize GABA directly in the gut.[8] These microbial metabolites send powerful "calming" signals to the central nervous system via the vagus nerve, immune, and endocrine pathways.[9]
This suggests that gut microbiome dysbiosis may directly impair the brain's GABA ergic system. Regulating the gut microbiome to boost GABA synthesis through the gut-brain axis may therefore represent a more fundamental solution.
Mechanism 3: The Overactive Stress Response System
Core Driver of Modern Insomnia: It’s not a brain chemical problem—it’s a stress hormone imbalance.
Feeling “tired but wired” at night comes from an overactive hypothalamic-pituitary-adrenal (HPA) axis, your body’s main stress system. Chronic stress keeps this system turned on, disrupting your cortisol rhythm — the hormone that wakes you up in the morning and should wind down in the hours before bedtime to allow restful sleep. When this fails, the amount of sleep you get decreases, and its quality suffers even more.
Research consistently shows that people with insomnia have elevated nighttime cortisol levels compared to healthy sleepers, a pattern documented across multiple clinical studies and confirmed by systematic review, pointing to chronic HPA axis hyperactivation as a core feature of the condition.[10]
Healthy vs. Stressed Cortisol Rhythms
Healthy Rhythm: Cortisol peaks at 7–9 a.m. to start your day and drops to its lowest between 2–4 a.m., letting you sleep deeply.
Stressed Rhythm: Chronic stress makes cortisol spike at night, keeping your body in a state of alertness.[10]
How Nighttime Cortisol Ruins Sleep
High nighttime cortisol harms your sleep in three key ways:
Blocks Melatonin: Cortisol stops melatonin from working, even if your receptors are healthy.
Kills Deep Sleep: High cortisol suppresses slow-wave sleep, leaving you with light, broken sleep.
Creates a Cycle: Poor sleep becomes a new stressor, making your body release more cortisol and worsening insomnia.[10]
Melatonin and GABA supplements are not designed to target the HPA axis directly. Resetting elevated nighttime cortisol requires interventions that address the stress response at its source, something standard sleep supplements are not built to do.[11]
Mechanism 4: The Anxious Brain’s Overactive Circuits
Sleep issues and anxiety are deeply intertwined — each making the other worse. About 80% of people with depression struggle with sleep, typically showing less NREM sleep, a faster transition into REM, and longer REM periods.[12] But the connection runs deeper than symptom overlap. Anxiety physically rewires the brain to stay alert, creating overactive neural circuits that no sedative can fully switch off.
Two Overactive Brain Networks
1. Alertness Network: The amygdala and locus coeruleus stay active in anxious people, keeping your brain on high alert. This makes you extra sensitive to noise or light, as your brain can’t turn off its “threat detection” mode.
2. Rumination Network: The default mode network, which handles self-reflection, forms strong links to emotional brain areas. This makes you fixate on worries at night, a physical brain issue, not just “overthinking.”[13]
Why Sedatives Don’t Fix the Anxious Brain
Traditional sleep aids and natural sedatives may make you drowsy, but they can’t target these overactive brain networks. They quiet overall brain activity but don’t turn off the specific circuits keeping you awake. The result is temporary sleepiness, not real relief from the anxious brain’s constant alertness. Unlike approaches such as cognitive behavioral therapy, which directly retrains sleep and stress response patterns, sedatives offer no lasting improvement in sleep quality for the anxious brain.[14]
Systemic Sleep Failure: When All Four Mechanisms Break
Chronic insomnia, especially from stress and anxiety, rarely comes from one broken system. It's a chain reaction:
Uncontrolled stress disrupts your cortisol rhythm, triggering HPA axis imbalance.
Chronic elevation of cortisol damages melatonin receptors, throwing your sleep-wake cycle off.
Ongoing tension depletes GABA and harms your gut microbiome, cutting off the brain's natural calming signals.
Stress and anxiety rewire the brain's neural circuits, locking you into a state of chronic over-alertness and rumination.

The result is a body with disrupted sleep signals, blocked calm pathways, a dysregulated hormone system, and an overactive brain. In this state, no single supplement, whether melatonin, GABA, or any other, can address the full chain of dysfunction driving chronic insomnia.
Final Thoughts: The Future of Sleep Formulation
For brands and product developers, the growing dissatisfaction with single-ingredient supplements is a clear market signal. To lead the next generation of the sleep wellness market, formulation strategies must go beyond the "one-size-fits-all" pill. They must adopt a "Systemic Repair" mindset.
The sleep supplement market, projected to reach $12.8 billion by 2035, is saturated with melatonin-only products that consistently fall short for consumers with stress-related or anxiety-driven insomnia. This gap represents a significant opportunity for innovation. Consumers are increasingly turning to herbal and natural supplements for sleep, yet improving sleep quality at a systemic level requires more than any single ingredient can deliver. An effective, science-backed formula must address the synergy between the four core biological systems:
Receptor Optimization: Moving beyond just adding melatonin to enhancing receptor sensitivity (MT1/MT2).
Gut-Brain Modulation: Utilizing advanced strains like Lp815 to trigger endogenous GABA production, bypassing the blood-brain barrier debate.
Endocrine Balancing: Formulating with ingredients that modulate the HPA axis to lower nighttime cortisol, addressing the "tired but wired" consumer.
Neural Circuit Calming: Targeting the hyper-arousal networks in the anxious brain to promote mental relaxation.
References
[1] Doghramji, K. Melatonin and Its Receptors: A New Class of Sleep-Promoting Agents. Journal of Clinical Sleep Medicine 3, (2007).
[2] Xie, Y. et al. (2025). Sleep disturbances in generalized anxiety disorder: The central role of insomnia. ScienceDirect / PubMed. https://pubmed.ncbi.nlm.nih.gov/40318600/
[3] ResMed. (2025). Resmed’s 2025 Global Sleep Survey [Webpage]. https://sleepsurvey.resmed.com/
[4] Gobbi, G. & Comai, S. Differential Function of Melatonin MT1 and MT2 Receptors in REM and NREM Sleep. Front. Endocrinol. 10, (2019).
[5] Ochoa-Sanchez R, Comai S, Lacoste B, et al. Promotion of non-rapid eye movement sleep and activation of reticular thalamic neurons by a novel MT2 melatonin receptor ligand. J Neurosci. 2011;31(50):18439-18452. doi:10.1523/JNEUROSCI.2676-11.2011
[6] Shen, W., Nan, C., Nelson, P.T., Ripps, H. & Slaughter, M.M. GABAB receptor attenuation of GABAA currents in neurons of the mammalian central nervous system. Physiol Rep 5, e13129 (2017).
[7] Hepsomali P, Groeger JA, Nishihira J and Scholey A (2020) Effects of Oral Gamma-Aminobutyric Acid (GABA) Administration on Stress and Sleep in Humans: A Systematic Review. Front. Neurosci. 14:923. doi: 10.3389/fnins.2020.00923
[8] Strandwitz, P. et al. GABA-modulating bacteria of the human gut microbiota. Nat Microbiol 4, 396–403 (2018).
[9] Grant, A.D. et al. GABA Probiotic Lactiplantibacillus plantarum Lp815 Improves Sleep, Anxiety and Increases Urinary GABA: a Randomized, Double-Blind, Placebo-Controlled Study. (2025) doi:10.1101/2025.04.14.25325830.
[10] Buckley TM, Schatzberg AF. On the interactions of the hypothalamic-pituitary-adrenal (HPA) axis and sleep: normal HPA axis activity and circadian rhythm, exemplary sleep disorders. J Clin Endocrinol Metab. 2005;90(5):3106-3114. doi:10.1210/jc.2004-1056
[11] Ring M. An Integrative Approach to HPA Axis Dysfunction: From Recognition to Recovery. Am J Med. 2025;138(10):1451-1463. doi:10.1016/j.amjmed.2025.05.044
[12] Yang SR, Lazarus M, Lu J. Editorial: The neural mechanisms involved in mood disorder-sleep disorder interaction. Front Psychiatry. 2025;16:1642372. Published 2025 Jun 25. doi:10.3389/fpsyt.2025.1642372
[13] de Lange et al. (2025). Multimodal brain imaging of insomnia, depression and anxiety symptoms indicates transdiagnostic commonalities and differences. Nature Mental Health.
[14] Balbo, M., Leproult, R. & Van Cauter, E. Impact of sleep and its disturbances on hypothalamo-pituitary-adrenal axis activity. Int J Endocrinol 2010, 759234 (2010).
[15] Future Market Insights. (2025). Sleep Supplements Market Outlook (2025 to 2035). Future Market Insights. https://www.futuremarketinsights.com/reports/sleep-supplements-market




































 Time:Jan 09, 2026
Time:Jan 09, 2026
 Share:
Share:











 +1(425)866-9043
+1(425)866-9043
 sales@bonerge.com
sales@bonerge.com